INTRODUCTION
Ultrasound guidance has become very popular for peripheral nerve block. Significant advantages over conventional nerve localization techniques include direct visualization of nerves and surrounding structures and local anesthetic spread, improvement in block quality, and increased patient satisfaction. It can also reduce the local anesthetic dose required for a successful block [
1], which might allow bilateral brachial plexus block to be performed without risk of local anesthetic toxicity. In addition, the use of ultrasound can detect normal and anomalous variations in nerve and vascular anatomy [
2,
3]. Subsequently, it might make needle adjustments to optimize local anesthetic distribution.
We present the case of a patient receiving a bilateral axillary block with ultrasound guidance and nerve stimulator, which revealed unilateral variant locations of the musculocutaneous (MC) nerve.
CASE REPORT
Consent for publication was obtained from the patient. A 38-year-old woman (height 152 cm, weight 79 kg, American Society of Anesthesiologists (ASA) physical status II) was admitted to our hospital for surgery of both carpal tunnel syndrome and right trigger thumb. Her medical history was remarkable only for medication-controlled hypertension. Preoperative laboratory evaluations were unremarkable. After a thorough discussion of risks and benefits with the patient followed by written, informed consent, ultrasound-guided bilateral axillary block with nerve stimulation was undertaken.
Standard ASA monitors were applied and supplemental oxygen delivered by facemask was administered throughout the procedure. Intravenous premedication (midazolam 2 mg and sufentanil 2.5 ╬╝g) was administered for anxiolysis. For simultaneous ultrasound-guided bilateral axillary block, a model 180 plus portable ultrasound machine equipped with a 5-10 MHz linear probe (SonoSite, Bothell, WA, USA) was used with nerve stimulation provide using a Stimuplex
® HNS 12 apparatus (B. Braun Melsungen, Melsungen, Germany). With the patient in the supine position, both shoulders were abducted and the elbows flexed. After skin disinfection and draping, the probe was placed in a vertical orientation at the axilla. Ultrasound scan in the right axillary region revealed no MC nerve in the coracobrachialis (CB) muscle (
Fig. 1). Using an in-plane technique and a lateral to medial direction, an insulated needle (UniPlex NanoLine, Pajunk
®, Germany) was advanced and directed toward a large nerve anterolateral to the axillary artery, which was presumed to be the median nerve. As the needle contacted the lateral part of this nerve, a MC nerve response (flexion of the elbow) was noted. The needle was then withdrawn and redirected above the nerve. A wrist flexion with 2
nd and 3
th finger flexion was produced when the tip of the needle reached above the medial part of this structure. Following negative aspiration for blood, 8 ml of 1.5% mepivacaine was slowly injected. Then, the radial and ulnar nerves located at the 7 and 8 oŌĆÖclock position relative to axillary artery, respectively, were identified and confirmed with a nerve stimulator. Four milliliters of 1.5% mepivacaine was deposited around each nerve. No swelling of the nerve or paresthesia to indicate intraneural injection was noted.
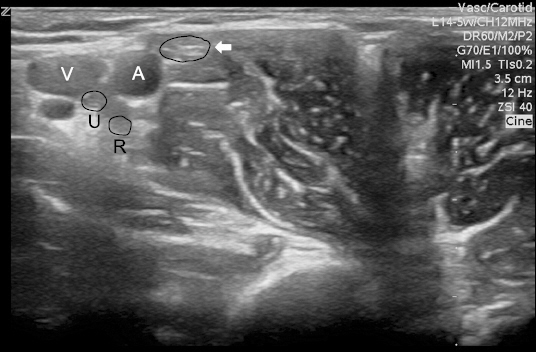
Fig.┬Ā1
Ultrasound image of right axillary region. The large structure (arrow) appears to consist of the musculocutaneous nerve and median nerve. Abbreviations: V = vein; A = artery; U = ulnar nerve; and R = radial nerve.
Immediately after the injection, the contralateral axillary block was started. Ultrasound scan of the left axillary region revealed the MC nerve in the CB muscle (
Fig. 2). The needle was directed to the muscle, biceps muscle contraction was elicited, and 4 ml of 1.5% mepivacaine was injected. The median, radial, and ulnar nerves were stimulated and the same dose of local anesthetic was injected in each. No swelling of the nerve or paresthesia was noted. Twenty minutes after receiving the second block, complete sensory and motor block of both upper limbs were confirmed. No symptoms or signs of systemic local anesthetic toxicity were noted.
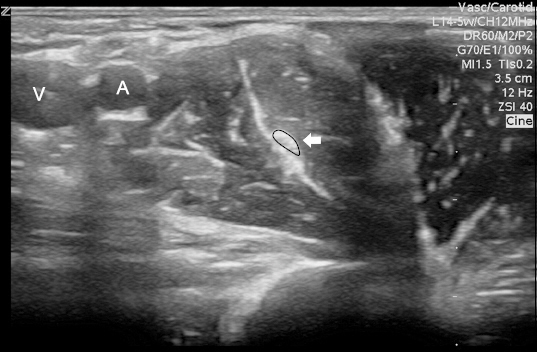
Fig.┬Ā2
Ultrasound image of left axillary region. The musculocutanoeus nerve (arrow) was localized between the coracobrachialis and biceps muscles.
Surgery was carried out uneventfully on both sides. In recovery room, she didnŌĆÖt complain any pain. The blocks wore off on both sides 3 hours later. No neurological deficits were identified at the follow-ups.
DISCUSSION
Anatomical variations of nerves and associated vasculature are extremely common and frequently observed during ultrasound-guided brachial plexus block [
4]. The most frequent anatomical variations found in the axilla are bifid axillary artery, multiple axillary veins, and variant location of the MC nerve [
5].
The MC nerve is a major peripheral nerve of the upper limb. It originates from the lateral cord of the brachial plexus. It normally pierces the CB muscle and then continues distally between the brachialis and the biceps brachii muscles, innervating both. In the elbow, it continues as the lateral cutaneous nerve of the forearm.
The MC nerve has frequent variations. The most common variations include the presence of abnormal connections between the MC and median nerves, absence of perforation of the CB muscle, and less frequently its absence [
6]. One study reported that communicating branches between the MC and median nerves were observed in 26.4% of the dissected arms [
7]. In another study, the MC nerve did not enter CB in 4% of the dissected arms [
6]. Two cases (8%) of absent MC nerve out of 24 dissected upper limb, with the innervations of the coracobrachialis, biceps brachii, and the brachialis muscles by branches of the median nerve were reported [
8].
In the axilla, the median, ulnar, and radial nerves are enclosed within the neurovascular sheath, while the MC nerve is usually separated from the other nerves. In addition, due to anomalous and collateral innervations of the arm, a standard triple-injection technique is superior to the selective injections at the nerves involved in surgery [
9]. Therefore, the MC nerve should be blocked separately to produce complete anesthesia of the upper limb in axillary block.
Although we did not measure the size of each nerve at the time of axillary block, it appeared that the size of the structure was the sum of the size of each nerve. In addition, both MC and median nerve responses were successfully elicited. Therefore, it is more likely that the MC and median nerves had been fused rather than complete absence of the former. Unfortunately, we did not distinguish these nerves after injection of local anesthetics due to the poor ultrasound image quality. The structure was also not followed with the transducer distally in the arm to verify its bifurcations. Thus, it is possible that the MC nerve was absent in the upper arm in this case.
The reported incidence of the MC nerve outside the CB muscle is 22% in axillary block [
10]. Similar to our case, variability of the MC nerve in the axilla ultrasound-guided axillary block has been described [
11]. In our empirical experience (unpublished data), the incidence of anatomical variation of MC nerve was 9.7% (3/31) during bilateral brachial plexus block. The three patients displayed similar anatomical characteristics as the present case. A thorough knowledge of the relevant anatomy and anatomical variations is essential for safe and successful regional anesthesia of the upper extremity. Failure to recognize this anatomical variation may lead to physician frustration during bilateral axillary block, especially for a novice. In addition, it may result in multiple needle passes seeking a MC nerve stimulation response, which might increase the risks for nerve injury, patient discomfort, or patient dissatisfaction. Use of traditional techniques may fail to detect such variations and potentially result in a failed block and/or unintentional neurovascular injury. In this case, we used a nerve stimulator during ultrasound-guided nerve block. Although use of a nerve stimulator does not influence the success rate during ultrasound-guided supraclavicular blocks [
12], we recommend it during ultrasound-guided brachial plexus blocks to identify the nerve, especially for a novice.
Bilateral brachial plexus block deserves mention. Bilateral brachial plexus block is generally considered a relative contraindication to bilateral upper limb surgery because of increased risks of technique-related complications and systemic local anesthetic toxicity. With conventional nerve localization techniques, large volumes and doses of local anesthetics are often used [
13], which might increase the risk of systemic local anesthetic toxicity. Furthermore, more proximal approaches have an increased risk of respiratory complications, such as pneumothorax and phrenic nerve block.
Axillary brachial plexus block is a commonly used technique for surgery below the mid-humerus. It is a safe and relatively easy technique. It can avoid the more significant adverse effects of the more proximal approaches due to its anatomical characteristics. In addition, one of several advantages of ultrasound-guided regional anesthesia is to reduce the local anesthetic dose required for effective blocks without side effects. Ultrasound-guided axillary block with low-dose local anesthetic can provide successful block for upper limb surgery [
14]. For this reason, we chose to use an axillary block for bilateral upper limb surgery. In this case, 32 ml of local anesthetic was used for bilateral brachial plexus block, representing half the conventional dose for traditional techniques.
In summary, we describe a case of ultrasound-guided bilateral axillary block in a patient with unilateral variant locations of the MC nerve. Use of ultrasound can allow practitioners to detect anatomical variants and perform a safe and successful bilateral brachial plexus block without unnecessary needle manipulations and risk of local anesthetic toxicity.
ACKNOWLEDGMENTS
This work was supported by Inha University Hospital research grant.
REFERENCES
1. Marhofer P, Schr├Čgendorfer K, Wallner T, Koinig H, Mayer N, Kapral S. Ultrasonographic guidance reduces the amount of local anesthetic for 3-in-1 blocks. Reg Anesth Pain Med 1998; 23: 584-8. PMID:
10.1016/S1098-7339(98)90086-4. PMID:
9840855.


3. Royse CE, Sha S, Soeding PF, Royse AG. Anatomical study of the brachial plexus using surface ultrasound. Anaesth Intensive Care 2006; 34: 203-10. PMID:
16617641.


4. Gutton C, Choquet O, Antonini F, Grossi P. Ultrasound-guided interscalene block: Influence of anatomic variations in clinical practice. Ann Fr Anesth Reanim 2010; 29: 770-5. PMID:
10.1016/j.annfar.2010.07.013. PMID:
20934304.


5. Berthier F, Lepage D, Henry Y, Vuillier F, Christophe JL, Boillot A, et al. Anatomical basis for ultrasound-guided regional anaesthesia at the junction of the axilla and the upper arm. Surg Radiol Anat 2010; 32: 299-304. PMID:
10.1007/s00276-009-0539-2. PMID:
19669074.



6. Uysal II, Karabulut AK, B├╝y├╝kmumcu M, Unver Dogan N, Salbacak A. The course and variations of the branches of the musculocutaneous nerve in human fetuses. Clin Anat 2009; 22: 337-45. PMID:
10.1002/ca.20734. PMID:
19090002.


7. Choi D, Rodr├Łguez-Niedenf├╝hr M, V├Īzquez T, Parkin I, Sa├▒udo JR. Patterns of connections between the musculocutaneous and median nerves in the axilla and arm. Clin Anat 2002; 15: 11-7. PMID:
10.1002/ca.1085. PMID:
11835538.


9. Sia S, Lepri A, Marchi M. Axillary block by ŌĆ£selectiveŌĆØ injections at the nerves involved in surgery using a peripheral nerve stimulator: a comparison with a ŌĆ£standardŌĆØ triple-injection technique. Reg Anesth Pain Med 2010; 35: 22-7. PMID:
10.1097/AAP.0b013e3181c6f395. PMID:
20052813.


10. Remerand F, Laulan J, Couvret C, Palud M, Baud A, Velut S, et al. Is the musculocutaneous nerve really in the coracobrachialis muscle when performing an axillary block? An ultrasound study. Anesth Analg 2010; 110: 1729-34. PMID:
10.1213/ANE.0b013e3181dc25c8. PMID:
20435937.


11. Orebaugh SL, Pennington S. Variant location of the musculocutaneous nerve during axillary nerve block. J Clin Anesth 2006; 18: 541-4. PMID:
10.1016/j.jclinane.2006.03.010. PMID:
17126786.


12. Beach ML, Sites BD, Gallagher JD. Use of a nerve stimulator does not improve the efficacy of ultrasound-guided supraclavicular nerve blocks. J Clin Anesth 2006; 18: 580-4. PMID:
10.1016/j.jclinane.2006.03.017. PMID:
17175426.


13. Kim BS, Kwak HS. Bilateral interscalene brachial plexus block for surgery on both upper extremities in a patient with unilateral vocal cord paralysis. Anesth Pain Med 2007; 2: 270-3.
14. OŌĆÖDonnell BD, Ryan H, OŌĆÖSullivan O, Iohom G. Ultrasound-guided axillary brachial plexus block with 20 milliliters local anesthetic mixture versus general anesthesia for upper limb trauma surgery: an observer-blinded, prospective, randomized, controlled trial. Anesth Analg 2009; 109: 279-83. PMID:
10.1213/ane.0b013e3181a3e721. PMID:
19535722.








